▼ Summary
– The JC virus is a common, lifelong infection that can become a rare, fatal brain disease called PML if it reactivates.
– The virus spreads via the fecal-oral route, with an estimated 50–90% of adults having been exposed, often asymptomatically in childhood.
– PML occurs when the dormant virus rearranges its genetic material and attacks brain cells, causing severe demyelination and neurological symptoms.
– The disease was historically rare but became an AIDS-defining illness, with a high fatality rate before effective HIV treatments were available.
– While modern antiretroviral therapy has reduced PML cases and mortality, survivors often suffer significant, lasting neurological damage.
A remarkably common virus, present in a significant portion of the global population, can transform into a devastating neurological threat under specific conditions. This pathogen, known as the John Cunningham (JC) virus, establishes a silent, lifelong infection in most people. However, when it reactivates and changes its form, it can trigger a rare but catastrophic brain disease. Recent research suggests a potential new pathway for this activation, raising fresh concerns about a virus many carry without ever knowing.
The JC virus, formally called human polyomavirus 2, was first identified over fifty years ago. It spreads through contact with contaminated waste, meaning infection often occurs early in life. Surveys indicate that exposure is incredibly widespread, with estimates suggesting between 50 and 90 percent of adults have encountered the virus. The initial infection is completely asymptomatic. The virus typically enters through areas like the tonsils or gut, then establishes a dormant, persistent state known as the archetype. For nearly everyone, this is where the story ends—a harmless passenger for life.
Tragically, for a small minority, the story takes a drastic turn. The dormant virus can reactivate and undergo a dangerous genetic rearrangement. This transformed, “PML-type” JC virus then travels to the brain, where it begins a destructive assault. It specifically targets cells responsible for producing myelin, the protective insulation around nerve fibers. This process, called demyelination, disrupts nerve signaling and leads to widespread brain cell death. The resulting illness is progressive multifocal leukoencephalopathy (PML).
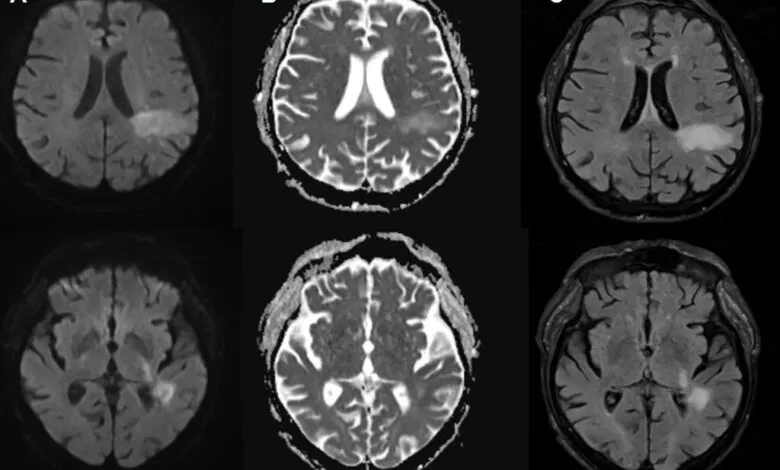
Diagnosing PML involves identifying characteristic lesions on brain scans and detecting the virus’s genetic material in spinal fluid. The symptoms, however, are notoriously variable and can be mistaken for other neurological disorders like stroke or multiple sclerosis. Patients may experience a rapid decline, suffering from speech difficulties, vision loss, impaired movement, and seizures.
Once considered exceedingly rare, PML gained notoriety during the HIV/AIDS epidemic. It became an AIDS-defining illness, affecting a notable percentage of patients before effective treatments existed. At that time, a PML diagnosis was almost invariably fatal. The advent of potent antiretroviral therapy in the mid-1990s changed the outlook, reducing cases and offering a chance of survival. Nonetheless, the disease often leaves those who recover with permanent neurological deficits. The discovery of a possible new activation mechanism underscores the need for continued vigilance regarding this stealthy viral inhabitant.
(Source: Ars Technica)